So I was on Total Parental Nutrion (TPN). Nicknamed Dracula food by Steve & me. We have loved having you the nurse said but your in demand, ward 107 want you. It’s only across the hall way. You don’t need to do anything. We are going to wheel your table, bed with you in it, and all your belongings. Paula and Esme took charged of my bed and my TPN. You have to be skill full in maouvering, especially when the there’s a patient like me hooked up to a feed and have a picc line in my arm, they are moving the bed and moving the pump stand . All went well. Paula made sure i had ice cold water; which she always did. Both ladies were very attentive in 106 I would miss the wee snippets of conversations or when you were feeling a bit down or needing something they would notice – I guess there will be staff in 107 that will be the same. Looking back the nursing in 106 wasn’t just physical support the emotional support was invaluable. When I had the episode of tissue oedema – Michelle was wonderful and spent time with me.
I’m in my new room of four. Hopefully I won’t be here too long. The other three beds had patients in them. The bed opposite – a lady in her 60’s: Susan, the bed beside her – a lady in her 50’s and the bed beside me had the curtains drawn with a lot of complaining.
It was the following morning I met my camp mates. The lady opposite – Susan – we became chums, helped each other, gave a willing ear to one another. The bed with the lady in her 50’s – we called the bed the lucky bed. Most people only stopped overnight in that bed. The bed beside me was quite another story. I nicknamed the patient “the gringe” – she was feeling miserable, had been in hospital for over 6 months. She said it herself in some ways she was desperate to get away from this place and in another way she felt safe and secure. Rather sad really.
The doctors/consultants/surgeons were the same as previous. Thank goodness Bev the dietician is still looking after me. She pops into the ward everyday, between one and three visits a day depending what there is to discuss. The nurses on the ward are all efficient, many of them are upbeat and help boost moral.
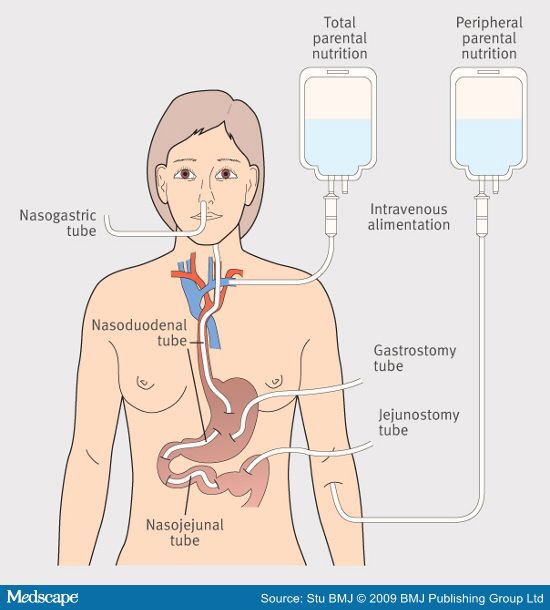
Day 11 of the Total Parental Nutrion (TPN) and I’m still leaking, the pain in my stomach doesn’t want to subside. The ward round is early this day, the usual gathering of doctors and surgeons round the bed. They examine me, listen to how I’ve been, they explain they would have something they would like try. Since I cannot get fed from the peg at the moment – even at at 10mls per hour it leaks. New plan put in an extension tube. The extension is called a jejunostomy feeding tube. It was to get put in that day in endoscopy. Cripes no waiting around.
So what’s the jejunostomy feeding tube? – The procedure was done down in endoscopy. Basically I was going to get a 6 foot very fine rubber tube inserted – it would go through my stomach and threaded through my intestines till it reached the jejunum. It will allow the feed to run through and go into me, It shouldn’t leak since the feed will be going a lot lower down.
The nurse comes over to me – “time to get you in a gown” she says, ” they will be taking you down soon”. She had to help me I’m still attached to the TPN – that’s not allowed to get disconnected, so one arm has the cable running to the Dracula food. She carefully and skilfully helps me manouevre out of my pjs and into the gown. At first it was all awkward, wondering which arm goes where, thinking about stuffing cables and large bag of feed into arm holes of tops, making sure everything is the correct way round and not inside out. Pjs off – gown on. All ready. I will go for a pea. Now I am ready.
The porter comes for me. The nurse has to come down with us, because I have TPN running. I’ve arrived. The staff are waiting on me.
I sign the necessary forms, get introduced to the four staff in the room. There are two doctors doing the procedure and two nurses assisting. First thing get a new cannula in. As ever it took a few attempts to get the cannula in, thankfully the doctor was a gem, she was gentle. All set for the sedation so I wouldn’t remember a damn thing 😴. Next came the delightful mouth spray – tastes of banana – really numbs the mouth and toungue. Then the nurse gently put on blood pressure cuff, sats monitor and oxygen. Then my least favourite – the mouth guard. It was carefully placed in my mouth and strapped. Then I was turned on my side. They were Blethering away to me, and said we are going to put the sedation in now. That’s the last I remember – thank goodness. Next thing that’s clear – truthfully is the next day. I know Steve visited me and my sister visited me – only because they told me.
We got the feed up and running. All attached and running. Bev recommended running at a low rate to begin with. So for the first 24 hours the TPN would still run, I would get goodness from two means, Once the rate was up and all running ok, I got the TPN down. The decision was to feed through the extension for 20 hours of 24 – giving me 4 hours of freedom. Ya beauty. This was the first time in four weeks I was not linked up to something for 24 hours per day. A step in the right direction. Big smiley happy face that day.
Bev had sorted the dietary requirements so I would be getting plenty of calories: the downside to this was changing the feed very late at night. One night. The nurse was doing my flush and putting up the feed. We heard a commotion behind the screen. It was Susan. She was buzzing to get up to the toilet. The CSW came to her, She was short and dumpy, perfect bobbed hair, although she waddled she actually looked like she floated. She was very cheerful, when she spoke to you no matter how you felt you couldn’t help but smile. She had a big heart and a big laugh. “how can I help sweetheart”? “I need the to go to the toilet and I can move – I’m strapped down to the bed” the little dark haired lady looked at her slightly puzzled, ” you daft moo your not attached to anything – think you have been dreaming” she said. She waddled away, chuckling to herself, you know it’s going to be a break time conversation. Small incidents like this kept me going.
I was in hospital for five weeks. Eventually. We had a feeding regime. I still had a painful tummy. And boy was it still leaking gastric contents. I asked how long would it take for it all to heal up. No one knew how long it would take. The time had come to take the big step. I was getting discharged. Home to our house. My own bed. Snuggle in with Steve – see my buddy & Bella. Smell the fresh air – oh yes can’t wait. It was four days later than originally planned, my discharge papers were done, meds done, Steve came to pick me up for 4pm. District nurses and GP phoned – organised for next day. Community dietician & consultant at western general phoned. All sorted. So excited 😀.

