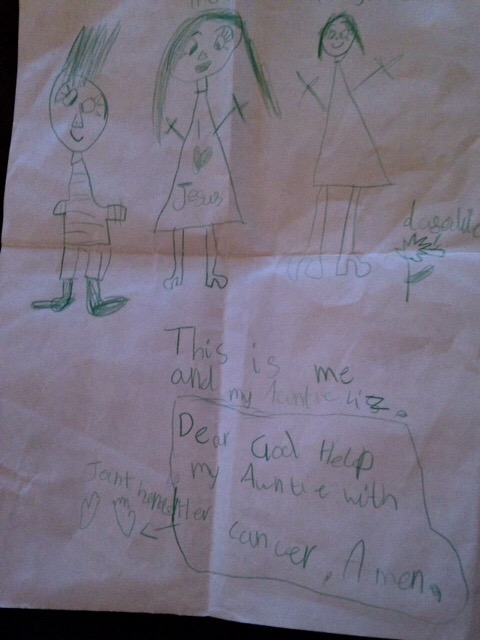The nurse and porter transferred me from the surgical obs unit ward to the surgical ward 106. I was put in base a in a room of 4 ladies. The staff were efficient and attentive and catered to every whim. They made sure I was comfortable and had my buzzer right beside me. All the strength that I once had seemed to have left my body. What used to be a simple task – getting out of bed, walking to the toilet, felt like a monumental task.
I needed someone to help me get comfortable, and get in and out of bed. I have graduated from the catheter to the commode and now walking to the toilet – woo hoo. Now I can walk to the bathroom with a stick in one hand and holding onto the arm of the nurse with the other.
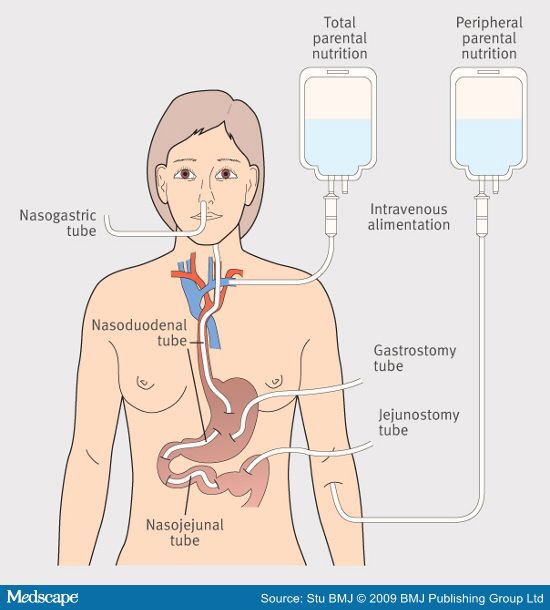
The next few days consisted of cleaning, dressings, obs, and pain relief. Most of it, I slept away. I was given triple intravenous antibiotics. The nurses on this base have been fabulous. I’ve had a 10% dextrose drip up to maintain my blood glucose levels. One of the awful symptoms of my carcinoid syndrome is spontaneous hypoglycaemia. My blood glucose level drops at a moments notice. The best way to avoid this is to keep something going into my body to elevated my glucose levels. Since my peg feed is leaking, there is no chance of feeding me through it at the moment – a glucose drip will at least keep my numbers up.
In the other three beds patients came and went and I was still there. I was so tired and sore I didn’t take too much notice of who they were.
With the exception of hubby Steve. Visiting in the first couple of weeks was kept short. One of my visitorsin base a was my precious niece Lindsay. She brought a picture and a story from her gifted daughter Sophie. Sophie was at church on the Sunday and asked if she could read out her prayer. She did. It was for me…..I don’t think there was a dry eye in the church. Sophie is seven years old.

So has came the day I’m moving from base A To base B. I’m graduating, 😀 now managing to wash myself with a basin – woo hoo. Actually the physical independence of being able to wash yourself is a fabulous feeling even if you feel you have just gone 10 rounds in the boxing ring. It takes five times as long to recover from getting washed as it did to actually get washed.
The room I moved into was friendly enough. There were two elderly ladies in their 80’s and a lady in her 50’s. We all got along. The lady in her 50’s was in the bed that changed people every few day The three of us were in the same room for two weeks. The three of us looked out for each other, pressed the buzzer for one another when needed, shared stories and shed tears. The three of us built up a friendship, that would last for at least the time in the hospital. We had our own system of communication and helping one another. When Mrs Mac struggled back from the toilet with her zimmer through the night and couldn’t get her oxygen back on, I would turn the torch on my phone shine it to her and guide her through the process of putting back on the nasal oxygen. Would then shine down to her slippers and she would use her stick to push them under her bed. When Rae couldn’t find her glasses we would shout over to her where they were. When I got up to go to the loo myself – they both would buzz – I would laugh and say do you think I need two nurses to take me 😀 ?
The one time the ladies really did help me was when they heard me swearing. I woke up my hair wet, the blue vest top clinging to my skin, beads of sweat running down my forehead. I went to lift my hand to press the buzzer and found I couldn’t lift my arm. It was a tonne weight. Using my other hand I searched around for my phone to try and shine a light. OMG all I could see was something that resembled a football shaped fist. My hand and arm was so swollen. My instant reaction…. “For fu*****” . Both ladies were instantly alarmed, put their lights on and called the nurse. The nurse came. Turned off the drip. Took out my cannula and called the doctor. I had tissue oedema. It was not pleasant. I had to get another cannula put in. The bad news for me is my veins keep collapsing, they look big and juicy and then disappear at a moments notice – naughty little blighters. After seven attempts the doctor got the cannula in. All this at 4am.
As all this was going on sometimes I find it hard to smile, the pain in my tummy, the endless leaking, the hypos……….
One evening around 10pm I’m feeling particularly homesick. My phone vibrates, I’ve got a video call from my hubby. It’s so wonderful to see our sitting room and our Labradors. I call their names, see their ear prop up, oh that’s my mums voice I can see in their face. I feel tears stream my face. Warm happy tears. What I would give to be on that sofa with them now.

We try a feed through my peg feed – just at 10mls per hour – bearing in mind my usual rate is 100mls per hour. Three hours later we look at the site – it’s wet. The 30mls have came out. Abandon feed. Bev the dietician comes to talk to me. She is a lovely lady. She has really kept me going. I get weighed – I’ve lost 5 kg – Bev says I’ve spoken to Mr Paterson-brown, I think the best thing is to put a picc line in and give you some TPN. TPN is a 24 hour feed directly into the veins. Steve and me call TPN Dracula food. It’s a Friday morning when they requested the picc line so I was told I may have to wait till the Monday. However, a young man comes to my bed at 12.45 and says hello there I’m here to take you for your picc line.
On the journey down to the cardiovascular lab to get my picc line inserted we met Mr Paterson-brown, he gently touched my shoulder and said “I’m pleased your getting the line in today Elizabeth, I will be up in the ward to see you in a while”. These good bedside manner from the doctors really help.
Oh wow entering the cardiovascular lab was something else. The staff were welcoming and chatty. There was quite a collection. A nurse, a radiographer, a radiologist and a technician. They were checking my date of birth and the radiographer said oh you are exactly two months younger than me. Oh dear, I’ve got the Devils child working on me. I looked at this beautiful lady, “you are only joking ” I say, she laughs reaches over to me and gently strokes my arm “I was born before the Omen came out” she whispers “I’m a genuine 666” we laugh together. One good thing it did do was make me feel relaxed. The nurse comes in, “come on you two bletherers lets get Elizabeth all set up”
The room has so many expensive technical machines. Absolutely fascinating. I get wheeled over to the bed. It’s rather high, I need a couple of steps to help me get up onto the bed. Once I’m on the long skinny bed the nurse straps me on securely. She puts the blood pressure cuff on my upper left arm and the sats monitor on my middle finger. ” I like to keep an eye on you at all times “she says. Up on a massive screen comes my name and all my readings. Yes, I have a pulse 😀. Thank goodness for that. Now for my right arm. It gets held down straight. The technician has a helmet on that looks like he is going to do some welding. He covers the majority of my arm with the green sheet, leaving an area of skin exposed. The radiologist then starts to do his work. After he introduced himself. His first words were just a scratch – why do they say that ? It’s never a scratch, he put the local anaesthetic in. He would use an ultrasound to guide the line up my arm, fiddle around via my armpit and guide it round to my heart. Fairly complex stuff. I needed more anaesthetic and it was more fiddly than he would have liked. But with his expertise he did a grand job and got it in. The X-ray machine came down approximately three inches above my chest. I tilted my head to the left, I could see my body on the screen, full chest X-ray with the picc line runnining from my mid left arm up to the arm pit and carrying along till it reaches the heart. WOW that’s ME. The nurse came round to my side, put a clear film dressing over the line. This dressing needs to be changed every week Elizabeth. She continued to take off the blood pressure cuff and sats monitor. And finally unstrapped me from the bed. She put the steps back to the bed for me to climb down. “Now take it easy” she gently said. My head was spinning, I took my time and gathered my thoughts. Gently does it girl. Down the steps and then over and onto my bed. The porter was waiting to take me back to the ward. When I got back I glanced at the clock, as I often did, it was 3.20pm. Gosh doesn’t time fly when you are having fun.
My Bear Hans keeping an eye on my picc line.
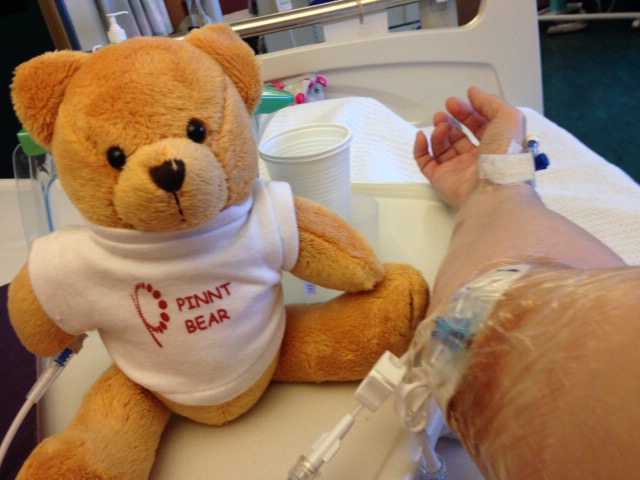
A few hours after getting my picc line in. Along came my lifesaving Dracula food. This is TPN – food fed through your veins 24 hours per day. Very clever really. The food is light sensitive and needs to be covered by a bag.
Here is Hans looking after my TPN

Once I was started on the TPN feed I had to get transferred to ward 107. My two ladies said they were going to miss me. Likewise I would miss them. The care I had in 106 was great – consultants coming round to see me at least twice a day, nurses looking after me very well.
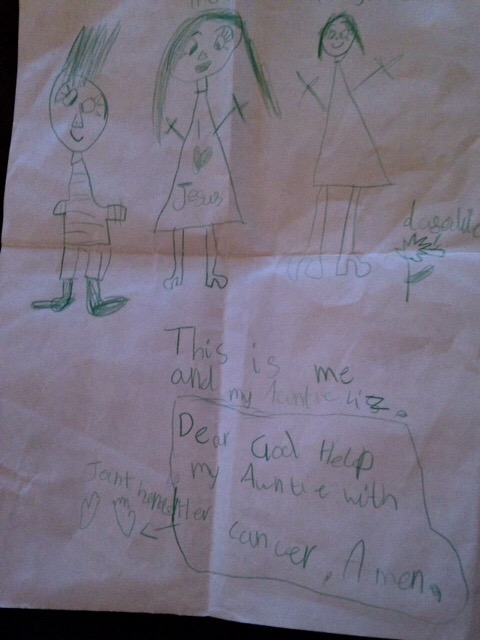
55.923430
-2.864864