July was met with a busy time including travelling to Suffolk to celebrate the wedding of steph and Levi. Five weeks later and we are returning to the same family – Adam (steph’s brother) is getting hitched to Elodie.
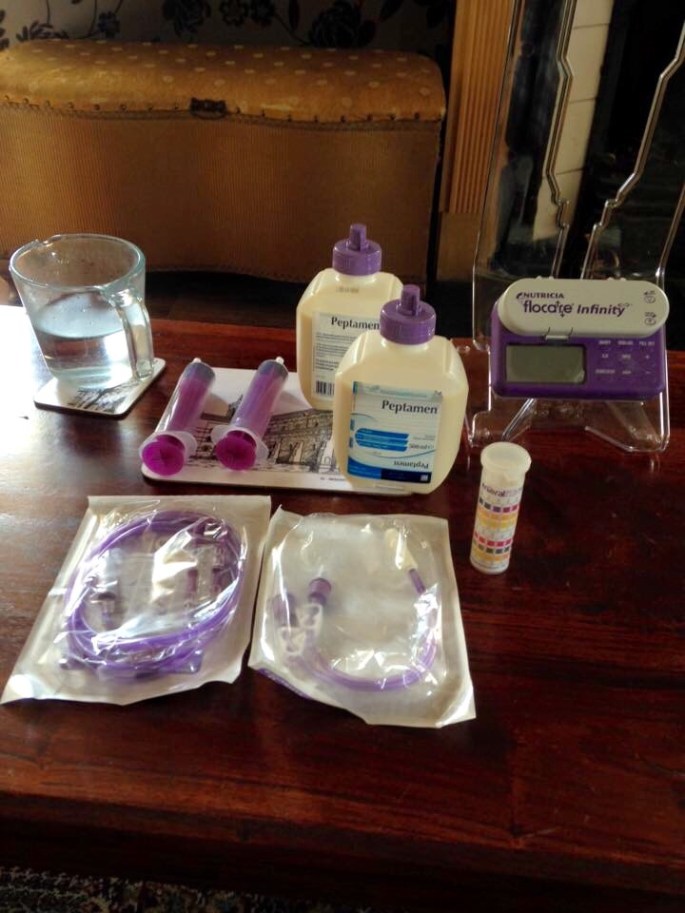
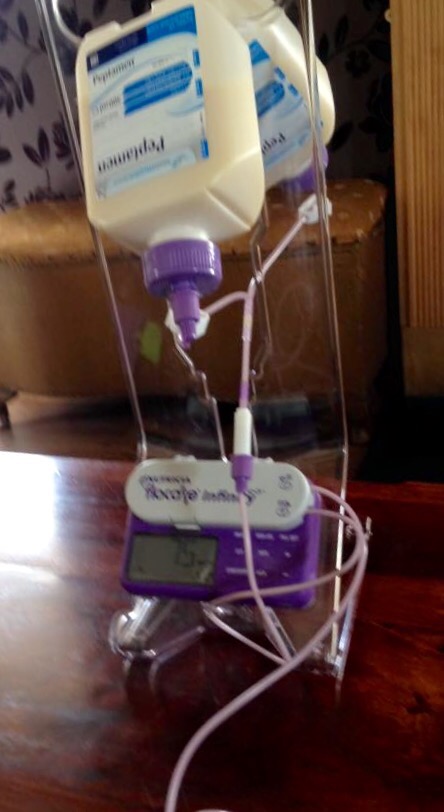
As usual it’s like a military operation to get organised to travel anywhere these days. Outfits chosen, suitable clothing packed in the case. Check and re check I have all my medication, creams, pump, milks, first aid kit, etc. And my companion bear – Hans. Could not possibly travel all that distance without my bear.

The nurse comes into our home on the morning we are heading down south. This is to check how I am and to do my dressings before heading off. My skin on my face, particularly where the tube had been resting has become agitated and red – some improvisation is needed: I’ve a cushioned dressing between the tube and my cheek now to prevent further damage. My nose where the plaster goes is getting red and a tad sore too. It’s all a little cumbersome but feels much more comfortable.
The day we travelled down was warm. Sun cream, hats, oakleys and the essential good playlist on the car hifi. Two hours short of our destination we make an essential toilet and coffee stop. On walking back to the car Steve gets stung by a wasp. In the matter of seconds his arm swells like a balloon. Fortunately we have cream with us to put on his arm. His singing is less enthusiastic and driving slower – I can tell his arm is very sore and he has been affected by the little blighter. We arrive at our destination. Anna has a lovely dinner on. We all tuck in and have a good natter. An hour later I’m more than ready for my bed. Pjs are on, feed pump is set up and all tucked in for the night it’s been a long tiring day.


Friday is the day before the wedding. Long lie, quiet morning then visit John and Sam in the afternoon. In the morning Steve rescued a bird, I was in my element taking photographs. Visit to John and Sam was lovely – really enjoyed it. In the evening Adam, the groom, had guests over – some friends, his cousin Megan and her husband Jason from Canada. Guitars were played, songs were sung, laughter filled the room. It was so lovely to see so many smiling faces. When Steve gets in bed he sees some flashing lights out of one of his eyes- we check the room – I assure him I can’t see any. Perhaps he is going to get a migraine.

So it’s Saturday and the day of the wedding. It’s also our 29th wedding anniversary. I can remember our wedding day so clearly. We have had our up and downs, but I have to admit I am happy to say that I still love the bones of that cocky young lad I met in high school who became my best friend, my lover, my husband, our two sons father, my rock. I can hear Steve talking about the day we got married – me on the back of his Honda cb350 the morning we are getting married to get a new pair of shoes. Four years ago I managed to get the very same bike for his silver wedding present.
This is Steve touching up his precious 25 year old bike.

Ahh such beautiful memories. Beep beep bong – that’s my 10 hour feed finished. Time to get up out of the bed. Disconnect myself from the pump. Get some boiled water. Draw it up the syringe. Flush my tube. Deteach the tubing and the empty bottle from the pump and stand. Dispose in recycling. Put pump on charge for later. Steve comes back into the bedroom armed with a welcomed cup of hot juice for me and to let me know he is heading out with the groom party for the ‘boys breakfast’. Just take your time he says you have been up several times through the night – last night was one of those nights that the bowels were in overdrive, the feed pump had a mind of its own and went off a couple of times…… I looked at Steve all dressed in his black watch kilt – yes I still love every inch of you. Probably more so than the day we married. The good news is Steve didn’t get a migraine, although his eye feels murky. He wants to eye drops – not like Steve at all. Fortunately our bedroom has an ensuite so off I toddle to get washed, apply my oilatum, then my diprobase cream over my whole body, then the factor 50 ultra sun sense sun cream. Phew – lie on the bed and have a wee rest. That’s one of the things that gets me the most – is the exhaustion. Words can’t describe the feeling of fatigue. I don’t like to sound like a moaning Minnie. It’s amazing how applying some cream to your skin can feel like a work out. I have taught myself to do things in stages and where possible out of the public eye. Ten minutes later and I’m ready to put on my Dundee cream (this is special sun reflectant coloured cream prescribed by a hospital in Dundee. It matches my colour tone, it reflects the sunlight and stops my skin burning. My skin reacts even in winter sun for as short as time as five minutes and can peel and blister when the light has shone through glass if I am not protected.) – the cream comes in two colours; coral pink and beige, I mix them together and apply it like foundation. Once it’s applied it looks great. Gives a healthy glow even on the peakiest days. Look at the watch – I’ve got a quiet hour before I need to get dressed. Anna and the girls are away to get their hair done.



Ta da we are all ready for the wedding – and what a lovely day it was too. I managed to stay till 10pm. But when Steve caught me sleeping at the table for the third time he insisted it was time for us to retire to our beautiful hotel room. I didn’t take any persuasion.
The Sunday and Monday were spent fairly leisurely, which was lovely. Feet up when we wanted, fun conversation, nostalgic conversation & some TV. Just what you need in preparation for a 400 mile journey home. Steve still kept rubbing his eye. He bought eye drops and put them in. He assured me he was ok, I wasn’t convinced. Looking forward to getting home and seeing our lads and our Labradors. And not to mention getting Steve’s eye checked out.
55.923522
-2.864845